Automate Benefits Workflows for Maximum Efficiency
Empower care coordinators to spend less time with phone calls and faxes, and delight people with quick activation of in-home services.
Here’s how it works:
- Build digital service provider networks for real-time visibility into capacity and availability.
- Efficiently broadcast service requests across your network.
- Complete service requests and track updates.
- Measure utilization to support compliance requirements.
More Than a Referral Engine
Built for efficiency, interoperability, and visibility, Dina’s care coordination solutions streamline network management, benefit coordination, and transitions of care.
Dina empowers teams to track patient and member progress with new home-based assessment data, and safely intervene throughout a person’s health journey via digital engagement tools.
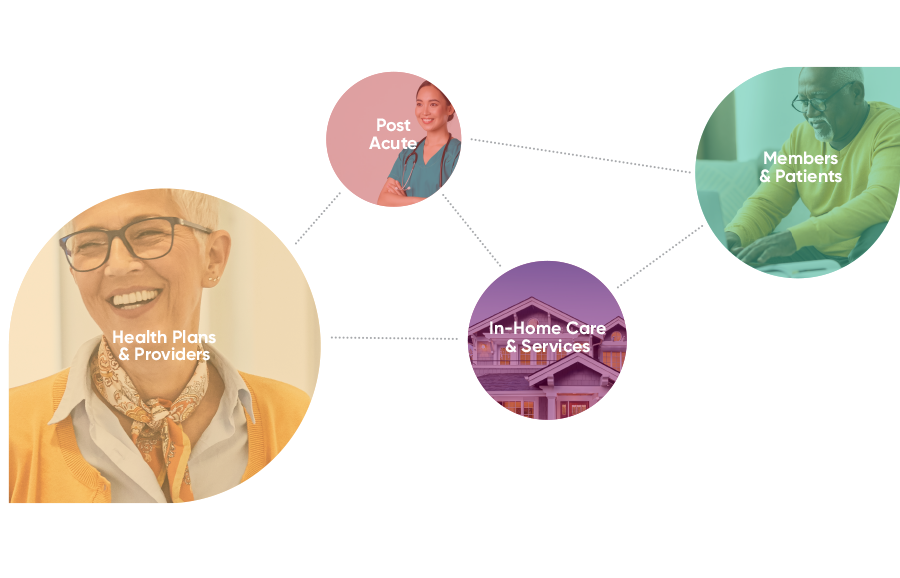
Care Traffic Control: Extend Coordination to the Home
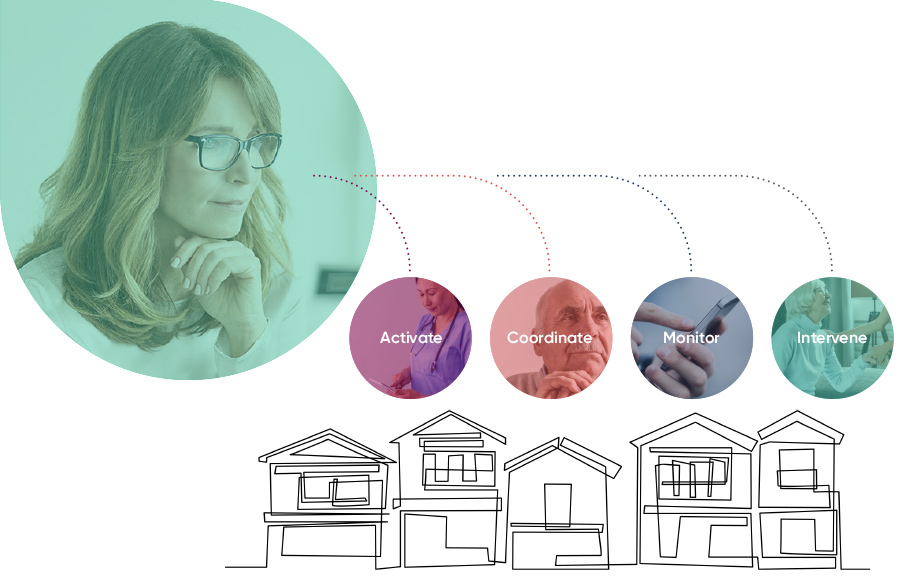
Using Dina’s “care traffic control” model, care navigators can coordinate benefits and home-centered services efficiently, and focus on those who are at risk of falling through the cracks.
Our care coordination solutions empower teams to manage care delivery throughout the journey, and remotely engage people to help them stay home safely. By leveraging home-based assessment data, care managers can identify risk and support the people who need it most.
Digitize Your Provider Network of In-Home Services
Personal Care & IHSS
Home Health
Hospice & Palliative Care
Respite Care
Home Modification Services
Medical Equipment
Medical Transport
Mental Health
Meals & Nutrition
Courier Services
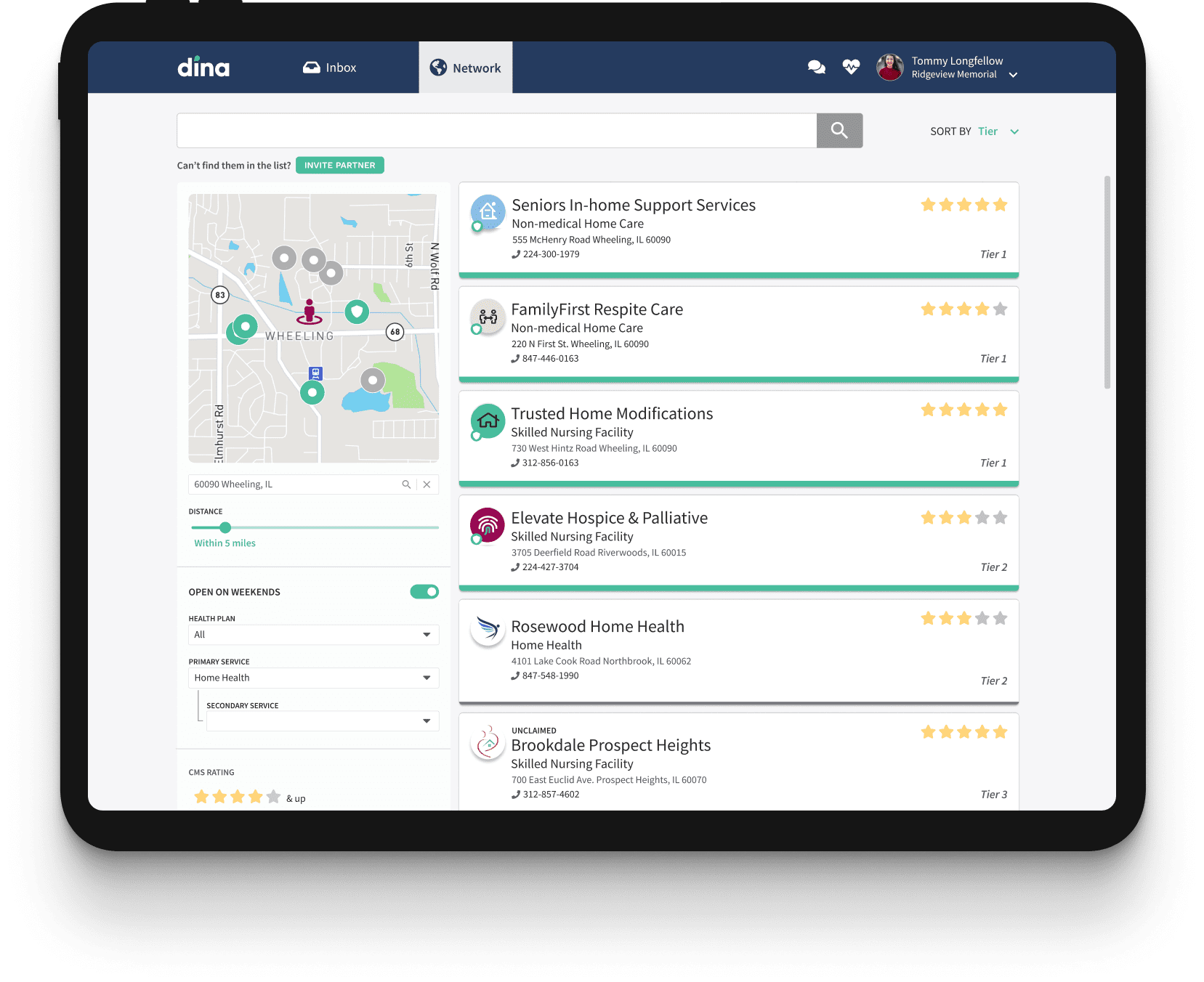
A New Perspective on Network Management
Leverage new types of data on engagement, responsiveness, and quality to continuously identify your highest-performing partners. Access comprehensive organization profiles to match members to appropriate resources. Structure your trusted network on the platform to reflect tiers, contracts and provider performance.
Reduce Costly
Healthcare Moments
To reduce costly healthcare moments like readmissions, avoidable hospitalizations, and ED visits, Dina’s technology goes beyond identifying the SDOH insights typically found in claims data or EHR records.
We close the loop on intervention management by leveraging proprietary algorithms and data sources to identify individuals who may benefit from additional home-based, or lower-cost care services.
Reduce Costly
Healthcare Moments
To reduce costly healthcare moments like readmissions, avoidable hospitalizations, and ED visits, Dina’s technology goes beyond identifying the SDOH insights typically found in claims data or EHR records.
We close the loop on intervention management by leveraging proprietary algorithms and data sources to identify individuals who may benefit from additional home-based, or lower-cost care services.

Powering In-Home Care Services
Health Plans
Digitally activate supplemental and other home-centered benefits for Medicare and Medicaid members to reduce administrative burden and improve member acquisition and retention.
Providers
Organize a safe landing home for people after an acute stay, including any in-home support, and remain connected to ensure they receive the care they need, when and where they need it.
Use Dina’s
Care Coordination Solutions to Power Your
In-Home Care
Increase in Coordination Efficiency
Services Coordinated
Network Partners
Used By Innovative Health Plans and MCOs





News & Insights
Learn more about connecting to one of today’s
most important care settings: the home.

Creating Value: Dina Unlocks Home-Based Benefit Delivery
First Analysis Managing Director Andrew Walsh is a longtime healthcare executive and entrepreneur, who has worked with organizations like Optum, UnitedHealth Group and DaVita Health. He founded and scaled Educerus Health Solutions (acquired by PopHealthCare), an...

MA Final Rule: Impact on Supplemental Benefits & Plan Growth
CMS released its much-anticipated 2025 Medicare Advantage (MA) and Part D final rule, codifying many of the provisions it proposed in the fall. We highlight six changes that will impact general enrollment MA plans, supplemental benefits programs, and D-SNPs, as well...

Health Related Social Needs Get Boost From Medicaid Guidance
Much like social determinants of health, addressing health related social needs (HRSN) is important for improving overall health outcomes and reducing health disparities. Several states are taking steps to address health related social needs and CMS is offering...

Moving the Needle on Outcomes Takes Center Stage at RISE National
The shift to value-based care and the role of health plans to support that vision was a key theme at the recent RISE National Conference in Nashville. “We continue to hear from benefit and in-home service providers about the importance of creating value and moving the...

Alignment, Growth Equity: How Medicare Can Propel Value-Based Strategy
CMS recently published an update on its Medicare value-based care strategy that anchors on three pillars: alignment, growth and equity. Notably, CMS calls on MA plans to use supplemental benefits to create value, and lean into the shift to value-based care. This call...

Policy Changes Don’t Damper D-SNP Growth
The D-SNP market continues to grow to accommodate the rapid rise of the dual-eligible population and ongoing policy changes from CMS that will shape the market. Beneficiaries who are dually enrolled in both Medicare and Medicaid are cited as a target pocket of growth...

Do You Know What Benefits Are Offered in Your Market?
Our team will analyze the counties or regions you operate in and share insights around the types of plans available, enrollment, and benefit portfolios. All at no charge to you.


